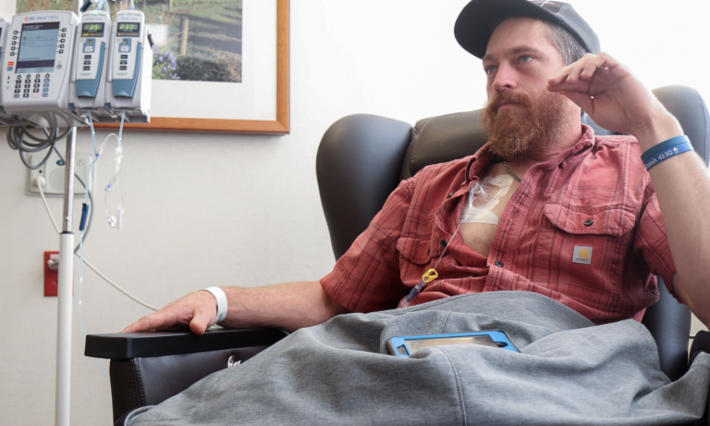
Elle Charnisky was the first patient accrued to the Duke-initiated "Mountaineer" study — a clinical trial for colorectal cancer patients with a HER2 amplification, which tested a regimen that included an FDA-approved breast cancer drug. She was a trailblazer. It worked. Below is HERstory and the HIStory behind her oncologist John Strickler's novel approach.

HERstory: Young Mom with Rectal Cancer Gets a Third Chance
Published
 From the Duke Cancer Institute archives. Content may be out of date.
From the Duke Cancer Institute archives. Content may be out of date.

Four years ago, Elle Charnisky had seven months to live.
"We were meeting with Dr. Tan, and I thought that it was a smart thing to do to ask what my prognosis was and he said something like, 'You know, when people have failed their third line treatment, it can be around seven months.’ And that kind of left my husband Mike reeling,” shared Elle, then a 37-year-old mother of two children under five. “The emotions were almost more there for him than for me, I think. I was just kind of putting one foot in front of the other, just doing what I needed to do… My husband had been the one to talk sense into me to even start chemotherapy treatment and everything. Now we were running out of options. It really hit him hard.”
That was June of 2017. Since her diagnosis of stage 4 rectal cancer in April 2016, Elle had been treated with the best standard-of-care therapies available. Her oncologist Benjamin Tan, MD, at Siteman Cancer Center in St. Louis, Missouri — one of the country’s best cancer hospitals and practically in her back yard — started her on FOLFOX (a potent chemotherapy combination of 5-FU, leucovorin, and oxaliplatin). Her original tumor nearly disappeared and the metastases in her liver and lungs got smaller. When Elle's cancer started growing again, her regimen was switched up to another chemotherapy combination, FOLFIRI — keeping the 5-
FU and leucovorin, holding the oxaliplatin, and adding irinotecan. It barely worked.
At diagnosis, Tan had encouraged the Charniskys to get a second opinion. Gastrointestinal oncologist Nancy Kemeny, MD, at Memorial Sloan Kettering Cancer Center — another top cancer center — became a key part of her care team early on. In February 2017, Kemeny had gotten Elle started on another regimen — irinotecan plus the EGFR inhibitor Vectibix (panitumumab) — an antibody drug that blocks the functioning of the epidermal growth factor receptor protein that’s thought to contribute to cancer cell growth. This third-line try was not the charm. Side effects were unmanageable and it didn't work at all.
“I got a weepy crusty skin rash and became very photosensitive,” recalled Elle. “I remember walking around my office building at lunch one day with a co-worker and the sunlight burned my eyelids through my sunglasses!
Elle would later reflect: “There were good weeks and bad weeks and we learned to live life in that way. I called it ‘life magnified’ because the bad times were much worse than we had ever experienced, but the good times were also so much better than they had been before. We had a newfound appreciation of life and we made sure to take full advantage of all the good stuff.”
Drawing Board
After that end-of-the-line meeting with Tan, they went back to the drawing board — seizing on the results of the molecular profiling tests of her tumor that Tan had ordered early on in case it opened up treatment options down the road.
The best-case option for patients for whom standard-of-care treatments have stopped working is the discovery, through molecular testing, of an actionable target — a specific aberration or mutation in the DNA of the cancer cells that drives their growth for which a drug has already been developed to home in on that target and slow its roll.
When patients develop resistance to treatment, it may mean their tumor has mutated and this new mutation could be "actionable." Even if it’s not, a new drug could emerge in the future that targets it. In the best-case scenario, the available drug is FDA-approved for the patient’s cancer. Next-best is if the patient can access the drug through a clinical trial that's recruiting patients OR if the patient can get the drug off-label for compassionate use.
Included on the list of Elle’s own cancer's many genetic characteristics was a HER2 amplification — found in the tumors of only 3 to 5% of metastatic colorectal cancer patients.
Normally, HER2 genes make HER2 receptors — proteins found in all cells of the body that help control how healthy cells grow, divide, and repair themselves. HER2 is said to be amplified in cases where the HER2 gene makes too many copies of itself, and it’s said to be overexpressed when the HER2 gene makes too many HER2 proteins. HER2 amplification or HER2 overexpression (or both) contribute to uncontrolled cell growth and division — cancer.
At the time, drugs aimed at stopping HER2 amplification or overexpression were only FDA-approved in HER2+ breast cancer and gastric/gastroesophageal cancer, though this mechanism had also been found, to varying degrees, to drive cancer-cell growth in the lungs, endometrium, bladder, gallbladder, and salivary glands.
Tan suggested they ask Genentech, the maker of one of the FDA-approved anti-HER2 drugs — Perjeta (pertuzumab) — if Elle could obtain the drug for compassionate use. The request was approved that July, but before she had a chance to obtain the drug, a call came in from Kemeny’s office asking Elle to come ASAP to New York and to bring the paperwork showing she was HER2+.
“It was funny, because you know, Dr. Kemeny’s amazing and super-efficient. And so, she brought us into her office, and we were in there for no more than five minutes. And she just pretty much said, ‘So you have this HER2 amplification?’ And I said, ‘Yes.’ And she said, ‘There's a guy at Duke, Dr. John Strickler, who I think you need to see. He’s working on a trial that I think would be perfect for you,'" recalled Ellle. "Then she said, ‘I'm going to have you go back out to my waiting room and wait for a call from his office.’ We told Dr. Kemeny that we were flying back to St. Louis the next day. And she said,‘Oh, good. So you can just go to Duke instead!’”
Strickler’s office called within minutes and in coordination with Kemeny’s office lined up an appointment for the next day. The couple scrambled to extend their childcare arrangements as they frantically searched for plane tickets.
They could only secure one plane ticket, so they hopped on an overnight train headed south that very night; pulling into Greensboro, North Carolina, at 2:30 a.m., then renting a car and driving to Durham later that morning for Elle's appointment with Strickler.
Right Place, Right Time
Since 2011, median survival for a metastatic colorectal cancer patient has been about two years, with only 16% of patients surviving five years.
Once a patient progresses past the third-line treatment, the available treatments (FDA-approved) even now add an average of only two more months of survival, Strickler explained in an interview with Duke Cancer Institute.
In Duke Cancer Institute's GI Oncology Clinic, six-plus years ago, metastatic colorectal cancer patients with a HER2 amplification were being offered another treatment option.
"Though it's rare, we were picking them up in the clinic, so I began treating these patients off-label with anti-HER2 drugs approved for breast cancer,” said Strickler, a GI oncologist and faculty co-leader of both the Molecular Tumor Board program at Duke Cancer Institute, and the Precision Cancer Medicine and Investigational Therapeutics Research Program at DCI. "Even though the breast cancer drugs provided some benefit, patients still experienced progression after a few months, and the side effects (diarrhea and rash) limited the ability to give a full dose."
At the time — around 2015 — a new generation of anti-HER2 therapies was being developed. These therapies appeared to offer enhanced inhibition of HER2, with fewer side effects.
“I said (to my colleagues), 'Look, there's some new breast cancer drugs coming out, why don't we go ahead and make a research partnership with a company making one of these drugs,’” recalled Strickler. “So, I wrote a proposal to a small biotechnology company in Seattle called Cascadian Therapeutics, and I said, ‘We should use your drug (tucatinib) and repurpose it for colorectal cancer because there's no FDA-approved options of these types of drugs in colorectal cancer.’ And they said, ‘Let's do it.’”
The multi-center phase 2 open-label trial – MOUNTAINEER — would test the efficacy of the experimental anti-HER2 drug Tukysa in combination with the well-established anti-HER2 drug Herceptin.
-
Tukysa, a tyrosine kinase inhibitor known in its elemental form as tucatinib, selectively blocks the HER2 signaling that promotes cancer-cell growth. At the time it was in clinical trials for metastatic breast cancer and already seeing success in that indication. (It wouldn’t be FDA-approved until April 2020 and then only in metastatic breast cancer)
-
Trastuzumab is a type of monoclonal antibody that binds to the HER2 protein and helps the immune system kill cancer cells. It had long been FDA-approved to treat advanced HER2+ breast cancer (1998) and had been approved around 2011 in HER2+ metastatic gastric cancer and HER2+ gastroesophageal junction adenocarcinoma.
-
In combination, the two drugs had been shown, in lab studies of HER2+ metastatic colorectal cancer (in patient-derived xenograft mouse models) and in clinical trials of HER2+ breast, gastric and gastroesophageal cancer, to work better together than separately to trigger tumor cell death.
Leap of Faith
By the time Strickler sat down with the Charniskys in early August 2017, he had just begun recruitment for MOUNTAINEER. He answered all their questions about the clinical trial. Since Elle would be in the first cohort of enrollees, she’d receive both drugs from the get-go.
An optimist by nature, Elle was ready to get started.
In his head, Elle's husband Mike replayed the life-expectancy conversation the Charniskys had had just two months before with Tan. He relayed his concerns to Strickler, who immediately put him at ease with "the promise of MOUNTAINEER."
“I was filled with a renewed sense of hope,” shared Mike. “The whole time my mindset has been that I will do anything and everything to find the right people, get to the right places and doctors to give my wife the best possible shot at longtime survival.”
Elle would be the first patient accrued nationwide — start-date August 8, 2017.
In just the first eight weeks, her carcinoembryonic antigen (CEA) level — which can be found at high levels in colorectal and other cancer patients — plummeted from 22 to 2.5 and continued to drop after that. The significant drop meant the trial drugs were working.
Elle's only side-effect was fatigue the day after the infusion. Compared to the grueling side-effects of chemo, including nausea and extreme fatigue, Elle shared, "it was as if all of a sudden I wasn’t even on treatment.”
Every three weeks, for nearly a year, she flew into Raleigh-Durham from St. Louis for her infusion and other appointments and returned back home the same day.
"It made for a really long day. And it was expensive,” said Elle.“We had talked about wanting to live closer to the beach and everything. And, after a while, we thought maybe we should move to the area. So, we did.”
Home Run
In June 2018, the family moved to the Research Triangle area, renting at first then committing to buying a house about a 40-minute drive from Duke and settling down. In January 2019, she went on disability.
With much more convenient access to her treatments and having left her job as an account manager at Equifax back in St. Louis, Elle was able to focus her energies on healing and preserving her strength. While she’d converted to Catholicism when she got married, it wasn’t until her cancer diagnosis that she became an avid Catholic; finding solace in the Church’s teachings, volunteering, and singing in the choir. She was also able to indulge her love of reading, and she became “addicted” to Spotify and podcasts.
Elle also got to spend precious time with her husband Mike and the kids, camping locally, visiting the North and South Carolina beaches, going to Walt Disney World, and celebrating milestones such as her son starting kindergarten. Her parents, who still lived in northeast Georgia where she’d grown up, were now closer-by and they visited often.
In fall 2019, two years into the trial, the MOUNTAINEER trial team, led by Strickler, presented preliminary findings at the 2019 European Society for Medical Oncology Congress in Barcelona, Spain. By that time, the trial had expanded to seven more sites nationally, including Dana-Farber Cancer Institute, Memorial Sloan Kettering Cancer Center, two Mayo Clinic sites, and a private practice clinic in Wisconsin.
Strickler reported that nearly 50% of participants on MOUNTAINEER had received a response. Having a "response” means there’s been a greater than 30% reduction in the sum of a patient’s cancerous lesions. That means half of those on the trial had a response according to this definition. And he reported that participants were surviving longer than they would have on standard therapies.
"While most patients are experiencing some benefit, we're seeing dramatic and durable benefit in about a third of patients,” Strickler explained, referencing the findings released publicly in 2019. “This is following a common pattern in cancer research. When the tumor is truly addicted to a genetic pathway, you can have a dramatic benefit from targeted therapy. Even in cases where there is short-lived benefit, the side-effects are such that most patients have an excellent quality of life while they're on it. Several patients have told me they feel so much better taking this combination compared to their past experience with conventional chemotherapy.”
Elle was one of those patients experiencing dramatic benefit. As Strickler put it, she was “hitting the ball out of the park.” For two and a half years on the trial, she would remain in full remission.

Critical Access
Elle and others with HER2+ metastatic treatment-resistant colorectal cancer were given the opportunity to participate in MOUNTAINEER because they knew from molecular profiling tests ordered by their doctors that their cancers had developed a-very-rare-for-colorectal-cancer HER2 amplification. Not all doctors order these kinds of tests and not all patients have this kind of access. Strickler sought to change this.
About a year and a half after MOUNTAINEER began enrollment, Strickler launched COLOMATE (COlorectal Cancer Liquid BiOpsy Screening Protocol for Molecularly Assigned ThErapy) through the Academic and Community Cancer Research United (ACCRU) trial network. This is a trial he designed to more quickly identify patients with HER2 amplification who could potentially benefit from clinical trials like MOUNTAINEER.
Launched in April 2020, participants are offered a simple blood test that looks for bits of DNA in the bloodstream shed by cancer cells (cell-free DNA) and screens this DNA for molecular aberrations that might be susceptible to a targeted therapy.
“Two tubes of blood are drawn from the patient. Within a week, the results come back and we see if we can match them to a trial,” said Strickler.
When the first patients began enrolling in COLOMATE, liquid biopsies, often used in lung cancer, were starting to be used with more frequency in GI cancers, though tissue biopsies were still the standard-of-care option. Early data had shown that liquid biopsies were often just as effective for detecting HER2 amplification.
COLOMATE was able to cast a wide net — across 18 sites nationally — to medically underserved colorectal cancer patients who would otherwise not have had access to molecular testing or the means to pay for it because they were either underinsured or not insured.
Duke Cancer Institute, for its part, was able to make the test available to this vulnerable population through its Research Triangle-based cancer clinics and through the Duke Cancer Network, a well-established academic-community partnership between DCI and 12 affiliate community treatment centers in the Southeast U.S., most of which are located in rural communities. These communities frequently report higher incidences of cancer and cancer-related deaths.
Despite the rarity of a HER2 amplification in colorectal cancer, the COLOMATE team has already identified several patients who might qualify for MOUNTAINEER. COLOMATE has also revealed other potentially actionable mutations in patients and has matched patients to several other trials.
Their Normal
Elle’s health continues to be monitored very closely with scans and bloodwork that regularly track her cancer and its side effects — the kind of surveillance that she said has been very reassuring. When there’s a new challenge, her care team is "right on it.”
In March 2020, her cancer recurred in the area where her original tumor took shape. Since it was caught early, it was small. Elle had never been eligible to have the primary tumor removed, but now with her cancer mostly under control and because she was so young and otherwise healthy, Strickler and radiation oncologist Manisha Palta, MD, advocated for surgery. The first person they asked to perform the surgery was GI surgical oncologist Julie Thacker, MD, and she agreed. Thacker removed the tumor and part of her colon that month. Elle had a temporary ileostomy, which was reversed that June.
Elle showed no further progression until the end of January 2021 when a CT scan picked up a small area in her liver that, upon inspection of past scans, appeared to be more pronounced each time. Toward the end of February after careful review and an MRI, DCI surgical oncologist Sabino Zani Jr., MD, a specialist in liver surgery, removed the approx. 1 cm lesion.
She didn’t have to come off the trial during either surgery.
"It’s very difficult to make breakthroughs in colorectal cancer. We opened the floodgates with MOUNTAINEER. We need to continue to get the word out that there's something more for these patients.” — John Strickler, MD
Life Magnified
This April, Elle celebrated her five-year anniversary of living with metastatic colorectal cancer.
Unfortunately, she had to come off the trial mid-month when her cancer recurred in her liver and lung.
"Elle played an active role in her care, communicating with the team, which helped to allay any fears she had,” said Leighanne Hartman, MSN, RN, AGNP-C, CHPN, CCRC, the clinical research nurse assigned to MOUNTAINEER for the first two years of the trial. She was an exceptional study patient, openly communicating with the research team, keeping us abreast of any new issues. We, as a team, provided reliable care and knowledge to Elle in the years we treated her, which instilled an invaluable trust and bond with her.”
Fortunately, coming off the trial didn't mean Elle was out of options.
She's proud of her role in MOUNTAINEER, grateful it worked as long as it did, pleasantly surprised by how her new drug combination (trastuzumab and pertuzumab) is working so far, and hopeful that she’ll qualify for a new anti-HER2 drug trial of the novel therapy trastuzumab deruxtecan — DESTINY-CRC02 — that launched last month at DCI.
"I'm a trailblazer," she said. “I'm hoping that sharing my story will help people.”
When Elle was first diagnosed, her son Grant was a one-year-old and Molly was four. Now they are six and nearly-10.
Having spent the past year navigating the pandemic, including the challenges of online school for the kids and two surgeries, life for the Charnisky family is starting to get back to their normal. Elle, 41, has begun reading the Little House on the Prairie book series with her kids. They’re enjoying their five-month-old puppy Louis, a whippet named after the city where their life as a family began. And they’re looking forward to more beach trips and other summer activities.
As a result of the success of her treatment on MOUNTAINEER and her natural ability to connect with others, Elle joined the Global Colorectal Cancer Association (GCCA) as a spokesperson for its Clinical Trial Awareness Program and Know Your Biomarker campaign. She's surprised when she hears from other colorectal cancer patients who don’t know their biomarker because they haven't had molecular profiling tests done.
“I’ve told people that you have to ask for that test and if your doctor isn't willing to order it for you, find someone who will because it can be life-saving,” she said.
In a taped interview with patient advocate and non-profit executive Martha Raymond, MA Ed. for the GCCA's Global Colorectal Cancer Congress 2021, Elle quietly and purposefully shared her cancer story, her wisdom, and lessons learned.
“I had always considered myself one of the healthiest people I knew,” Elle began … She went on to matter-of-factly describe a more than eight-month progression of warning signs for rectal cancer she missed — from intermittent mucous-y discharge and unusual constipation to dark blood in her stool, to a premature straining feeling when she went to the bathroom — confounding symptoms neither she nor her primary care doctor attributed to cancer right away since she was still in her thirties and couldn't recall any associated family history. That is until her primary care doctor explored her lower colon with a flexible sigmoidoscopy and found a rectal cancer tumor that had already metastasized to her liver and lungs.
The rest is HERstory ...
Learn More
According to a colorectal cancer trends report in the journal Cancer, patients diagnosed with with colorectal cancer who were younger than 50 were more likely to have primary rectal cancer vs primary colon cancer, and were more likely to have stage 3 or stage 4 disease at diagnosis.